How Much Does a Liver Transplant Cost?
Last Updated on February 20, 2024
Written by CPA Alec Pow | Content Reviewed by ![]() CFA Alexander Popinker
CFA Alexander Popinker
A liver transplant is a complex, life-saving surgical procedure that comes with considerable costs. With the average liver transplant costing anywhere from $200,000 to $890,000 in the United States, it is important for patients to understand the factors that influence pricing and strategies to manage expenses.
This article provides an in-depth analysis of the costs involved at every stage of the liver transplantation process.
The liver is a critical organ that performs vital functions like filtering toxins and waste from the blood, producing proteins, and metabolizing nutrients. When the liver fails due to disease, a transplant may be necessary to save a patient’s life.
Because of strict regulations around organ allocation and the intensive medical care required, a liver transplant is one of the most expensive transplant procedures.
How Much Does a Liver Transplant Cost?
With the average liver transplant costing anywhere from $200,000 to $890,000 in the United States, it is important for patients to understand the factors that influence pricing and strategies to manage expenses.
Medical News Today notes that in 2020, a liver transplant cost around $878,400 for procurement, procedure, and aftercare. Insurance can often cover much of the cost, and some organizations can provide financial aid.
According to Flymedi, the average liver transplant cost is highly variable and dependent on the patient’s health, age, the hospital where the procedure is done, and the region in which the hospital is located. The average liver transplant is around $600,000 or more in the United States, including follow-up care and medications after the procedure.
Breakdown of Liver Transplant Expenses
The overall cost of a liver transplant can be divided into three phases: pre-transplant evaluation and waitlist period, the transplant procedure itself, and post-transplant follow-up care and medication. Each phase comes with its own costs from multiple providers.
Pre-Transplant Costs
Once diagnosed with liver failure, patients will need to go through an extensive set of tests, scans, consultations, and procedures to determine eligibility for transplant.
- Initial evaluation – includes bloodwork, imaging, cardiac testing, psychosocial evaluation, nutritional assessment, etc. Cost is $2,000-$4,000 with insurance coverage.
- Waitlist registration – involves legal and data coordination fees to get listed on the national organ transplant waitlist. Typically costs $1,500-$2,000.
- Continued screening – requires frequent lab work and scans while waiting for a donor organ. Expenses vary based on the length of waitlist stay.
- Transplant coordination – involves regular consultations with the transplant coordinator to manage the process. Costs depend on transplant center fees.
Transplant Procedure Expenses
The surgery and hospitalization portion involves high costs from surgeon fees, operating room charges, and inpatient care.
- Surgeon’s fees – average $150,000 depending on the transplant center.
- Operating room charges – approximately $50,000. Cover staffing, and equipment costs.
- Hospital stay – usually 1-2 weeks. Around $150,000 with medications.
- Blood work – frequent lab tests during hospitalization averaging $3,000-$6,000.
Total transplant procedure expenses range from $300,000 to $400,000 on average.
Post-Transplant Follow-Up Costs
After a liver transplant, meticulous medical care and medication are vital to prevent organ rejection.
- Hospital readmissions – for complications like infections or rejection episodes. Adds $15,000-$30,000 per hospitalization.
- Medications – anti-rejection drugs needed lifelong can cost $2,500-$5,000 monthly.
- Frequent lab work – blood tests for medication monitoring average $2,000-$3,000 monthly.
- Follow-up visits – regular consults with the transplant team. Around $500 per visit.
- Transplant program fees – covers coordination of post-op care – $1,500-$3,000 yearly.
Factors Influencing Liver Transplant Costs
Several key factors lead to pricing variations for liver transplants across different hospitals and geographical locations.
Donor Type
- Living donor transplant – $285,000 to $530,000 on average. Involves lower wait times but added donor evaluation costs.
- Cadaveric donor transplant – range from $350,000 to $890,000. Waitlist time can drive up pre-transplant expenses.
Transplant Center
Location, specialists, and amenities at the transplant center influence pricing. Academic centers often charge higher fees. Centers performing large transplant volumes tend to have better rates negotiated with payers.
Geography
Considerable variation exists between regions, states, and cities. Costs in the Midwest or South are generally lower than either coast. New York City or San Francisco can average above $600,000 while an area like Cleveland may be around $350,000.
Insurance Status
Government insurance like Medicare and Medicaid provide the highest coverage with more pricing regulation compared to private plans. Uninsured patients may be charged 2-3 times more than insured individuals.
You might also like our articles about the cost of a kidney, anesthesia, or blood transfusions.
Insurance Coverage and Out-of-Pocket Expenses
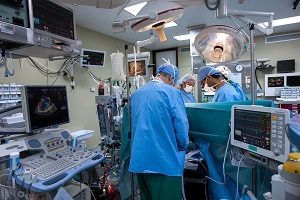 Health insurance plays a major role in financial preparedness for transplant. However, even insured patients can face high out-of-pocket costs.
Health insurance plays a major role in financial preparedness for transplant. However, even insured patients can face high out-of-pocket costs.
- Deductibles need to be met before coverage kicks in. Can be $2,000-$10,000 for private plans.
- Lifetime limit may cap total payouts below the full transplant cost. Government insurance has no lifetime maximum.
- Coinsurance of 10%-30% still applies for all in-network services.
- Out-of-network hospitals lead to substantially higher copays or no coverage.
- Prescription copays add up for medications post-transplant.
- Non-medical costs like lodging, food, or lost wages are generally not covered.
Without careful planning and supplemental funding, out-of-pocket expenses can easily exceed $50,000-100,000 for a liver recipient.
Financial Assistance and Support Services
Reputable resources exist to aid under and uninsured patients in managing transplant expenses:
- Hospital charity care programs – provide fee reductions or forgiveness based on income.
- State Medicaid programs – may offer low or no cost coverage options.
- National Foundation for Transplants – provides fundraising assistance.
- American Liver Foundation – offers co-pay relief and medication assistance.
- HealthWell Foundation – grants financial aid for prescriptions.
- HelpHopeLive – raises transplant funds through community outreach.
Strategies for Managing Liver Transplant Costs
For patients undergoing a liver transplant, effective budgeting and utilization of resources is essential to limiting out-of-pocket expenses:
- Have savings to pay deductibles and medication copays. Government insurance requires less upfront costs.
- Pick an in-network transplant center and negotiate self-pay rates if uninsured.
- Enroll in prescription assistance programs from drug manufacturers.
- Use supplemental insurance, Medicaid, or Medicare for coverage gaps.
- Set up a fundraising campaign and apply for medical grants.
- Discuss costs upfront with financial coordinator and eliminate unnecessary tests or procedures.
- Compare prices between hospitals to find lower-cost options.
Final Words
While a liver transplant can cost over $500,000 on average, options exist to curb expenses through careful planning and financial assistance. Controlling out-of-pocket costs involves due diligence across all stages – from choosing the right transplant center and supplementing insurance to budgeting for lifelong medications.
With thorough preparation and utilizing all available resources, the financial burden of this lifesaving treatment can be managed.
Frequently Asked Questions
Is it free to have a liver transplant?
No, a liver transplant is not free. The total costs range from $200,000 to $890,000 on average. Some components may be covered by health insurance, but patients still have to pay deductibles, copays, and other out-of-pocket expenses that can exceed tens of thousands of dollars without proper financial planning.
Government insurance like Medicare and Medicaid provide the highest coverage. Uninsured patients can negotiate discounted rates and apply for financial assistance. But liver transplants still incur considerable medical bills.
How risky is a liver transplant?
A liver transplant surgery carries moderate risks. According to recent data, the survival rate is quite favorable but complications can occur. Within the first year after liver transplant, 15% of patients may experience acute organ rejection and up to 10% may pass away. The risk of blood clots, infections, and post-operative bleeding is between 5-10%. Over the long-term, the most common causes of death are cardiovascular disease and malignancies from immunosuppression.
However, with careful monitoring and management, many transplant recipients can expect to have good functional outcomes and quality of life after the surgery. The risk profile continues to improve with advances in organ matching, surgical techniques, and post-transplant care.
Can we donate liver while alive?
Yes, it is possible to donate a portion of the liver while alive. This is called living donation and accounts for about 1/3rd of all liver transplants. The liver’s unique ability to regenerate allows a healthy person to donate up to 50% of their liver safely.
Typically, the right lobe is transplanted to an adult recipient. Donors undergo extensive medical and psychosocial evaluation to ensure it is safe for them to donate. While serious complications are rare, common donor risks include pain, hernia, bile leaks, and blood clots after the surgery. Living liver donation is an option for patients who cannot wait for a cadaveric donor transplant. However, donating requires the donor to undertake permanent health risks, even if minimal.
Who Cannot donate a liver?
Some medical conditions and behaviors disqualify a person from donating their liver. Ineligibilities include:
- Untreated infections like hepatitis B or C, HIV
- Active alcohol or drug abuse
- Severe obesity with a BMI over 35
- Uncontrolled diabetes or hypertension
- Significant heart or lung disease
- Vascular abnormalities of the liver
- Hematologic disorders
- Autoimmune disorders
- Liver disease or cancer
- Psychiatric conditions impacting consent capacity
- Age over 60 years in most cases
Careful screening is done to ensure only healthy individuals without increased surgical risks choose to donate. Certain medications, previous surgeries, or allergies may also limit eligibility. The transplant team determines if liver donation is safe on a case-by-case basis.
What is the age limit for a liver transplant?
There is no strict age limit, but most transplant centers follow guidelines to determine patient selection criteria. Infants as young as 6 months have received liver transplants, while the oldest recipient was over 90 years old. The guidelines consider:
- For children under 10 years old, long-term graft survival rates are excellent.
- Teenagers and young adults in their 20s and 30s have the best outcomes. Their youth helps them recover and tolerate anti-rejection medications well.
- Middle-aged and older adults in reasonably good health can still do well with a liver transplant. Cases are evaluated individually.
- Patients over age 70 are at higher risk but may still be candidates depending on their comorbidities and functional status.
While age does impact transplant eligibility, recipients of all ages can benefit. The key factors are the person’s overall health condition and expected survival rate with and without a new liver.


Leave a Reply
Want to join the discussion?Feel free to contribute!